Start Here: Reset Your Metabolism
If you want a structured starting point, download our free 7-day metabolic reset guide.
A simple, clinically-informed plan to help stabilise blood sugar, improve metabolism, and reduce common PCOS symptoms.

What Is PCOS
Polycystic Ovary Syndrome (PCOS) is a common hormonal condition affecting up to 1 in 10 women of reproductive age.
It is typically diagnosed based on a combination of:
- Irregular or absent menstrual cycles
- Elevated androgen levels (male hormones)
- Polycystic-appearing ovaries on ultrasound
While these are the defining features, they don’t explain why PCOS develops—or why symptoms vary so widely between individuals.
This is where metabolic health becomes critical.
Emerging evidence shows that for a large proportion of women, PCOS is closely linked to underlying metabolic dysfunction, particularly involving how the body processes and responds to insulin.
How PCOS Affects Metabolism
Metabolism refers to how your body converts food into energy and regulates key processes such as blood sugar, fat storage, and hormone balance.
In PCOS, several metabolic processes become disrupted.
Most notably:
- The body becomes less responsive to insulin
- Blood sugar regulation becomes less stable
- The body is more prone to storing fat, particularly around the abdomen
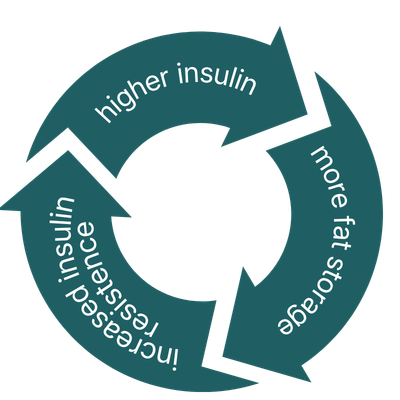
These changes can create a cascade effect:
- Increased insulin → increased androgen production
- Increased androgens → disrupted ovulation and symptoms
- Ongoing imbalance → worsening metabolic function over time
This is why many women with PCOS feel like their body is “working against them” - because at a metabolic level, it often is.
Over time, this cycle makes it harder to:
- maintain a healthy weight
- feel energised
- regulate appetite
The Role of Insulin Resistance in PCOS
Insulin resistance is one of the most important - and often misunderstood - drivers of PCOS.
Understanding how it works is key to improving both metabolic health and PCOS symptoms.
What is Insulin Resistance?
Insulin resistance occurs when the body’s cells become less responsive to insulin.
As a result:
- The body needs to produce more insulin to achieve the same effect
- Blood insulin levels remain elevated
- Blood sugar becomes harder to regulate
Over time, this can lead to fatigue, cravings, weight gain, and increased risk of metabolic conditions.
Why Is Insulin Resistance Common in PCOS?
In PCOS, insulin resistance is extremely common—even in women who are not overweight.
Higher insulin levels stimulate the ovaries to produce more androgens (male hormones), which contributes to symptoms such as:
- Irregular cycles
- Acne
- Excess hair growth
At the same time, elevated insulin promotes fat storage and makes weight loss significantly more difficult.
This creates a cycle: Insulin resistance → hormone imbalance → worsening metabolic function
Struggling with symptoms that don’t make sense?
If insulin resistance is driving your PCOS, the right strategy can make a significant difference.
Download the PCOS Metabolic Reset Guide to learn how to stabilise blood sugar and support your metabolism step-by-step.
Does PCOS Slow Your Metabolism?
This is one of the most common - and most frustrating - questions women with PCOS ask.
The short answer is: PCOS doesn’t directly “break” your metabolism, but it can significantly impair how efficiently it functions.
In clinical practice, what we often see is not a damaged metabolism, but a dysregulated one.
With PCOS:
- Insulin resistance makes it harder for the body to use glucose effectively
- Elevated insulin levels promote fat storage
- Blood sugar fluctuations can impact energy levels and appetite
This combination can create the feeling of a “slow metabolism,” even when calorie intake and activity levels haven’t changed significantly.
For many women, this shows up as:
- Gaining weight more easily
- Struggling to lose weight despite effort
- Feeling fatigued or sluggish throughout the day
The key insight here is that improving metabolic function—not just reducing calories—is what creates meaningful change.
Why PCOS Can Lead to Weight Gain
Weight gain with PCOS is not simply a matter of willpower or lifestyle choices—it is often driven by underlying metabolic and hormonal factors.
When insulin levels are elevated:
- The body is more likely to store energy as fat
- Fat breakdown becomes less efficient
- Hunger and cravings—particularly for carbohydrates—can increase
At the same time, hormonal imbalances can further complicate things:
- Higher androgen levels can affect fat distribution
- Disrupted ovulation can influence appetite and energy regulation
This is why many women feel stuck in a cycle: “I’m doing all the right things, but nothing is changing.”
From a metabolic perspective, the body is being signalled to store energy rather than use it efficiently.
Until that signal is addressed, weight loss can feel unnecessarily difficult.
Common Metabolic Symptoms of PCOS
While PCOS is often discussed in terms of reproductive symptoms, many of the day-to-day challenges women experience are actually metabolic.
These symptoms can vary, but commonly include:
- Persistent fatigue, even after adequate sleep
- Strong cravings for sugar or refined carbohydrates
- Energy crashes, particularly mid-afternoon
- Difficulty losing weight, or unexplained weight gain
- Increased abdominal fat storage
- Feeling “shaky” or irritable when meals are delayed
These are often signs that blood sugar regulation is not stable.
Recognising these patterns is important, because they point to where intervention can be most effective.
Blood Sugar Imbalance in PCOS
Blood sugar regulation plays a central role in metabolic health—and in PCOS, it is often disrupted.
When blood sugar rises quickly (for example, after a high-carbohydrate meal), the body responds by releasing insulin.
In insulin resistance:
- More insulin is required
- Blood sugar may drop more rapidly afterwards
- This can trigger hunger, cravings, and energy dips
Over time, this pattern can become a cycle:
👉 Blood sugar spike → insulin surge → energy crash → cravings → repeat
This cycle doesn’t just affect energy—it also contributes to hormonal imbalance and ongoing metabolic dysfunction.
Stabilising blood sugar is therefore one of the most effective ways to begin improving both metabolism and PCOS symptoms.
Nutrition Strategies to
Improve PCOS Metabolism
The encouraging part is that metabolic function is not fixed—it is highly responsive to the right inputs.
Rather than focusing on restriction or extreme approaches, the goal is to support the body’s ability to regulate blood sugar and insulin more effectively.
In practice, this usually involves a combination of:
1. Prioritising Protein Intake
Protein plays a key role in satiety, muscle maintenance, and metabolic activity.
For many women with PCOS, increasing protein intake can:
- Reduce hunger
- Support fat loss
- Improve blood sugar control
2. Structuring Meals to Stabilise Blood Sugar
Balanced meals that include protein, healthy fats, and fibre help slow glucose absorption and reduce insulin spikes.
This can lead to:
- More stable energy
- Fewer cravings
- Improved metabolic efficiency
3. Reducing Reliance on Refined Carbohydrates
Highly processed carbohydrates can lead to rapid spikes and crashes in blood sugar.
This doesn’t mean eliminating carbohydrates entirely—but rather choosing sources that support more stable energy.
4. Consistent Meal Timing
Erratic eating patterns can worsen metabolic instability.
Aim for:
- regular meals
- avoiding constant snacking
- structured eating windows
5. Supporting Consistency Over Perfection
One of the biggest shifts is moving away from short-term diets toward consistent, sustainable habits.
Metabolic improvements happen over time, not through extreme restriction.
If you’re unsure where to start…
The PCOS Metabolic Reset Guide walks you through exactly how to structure your meals and stabilise your metabolism in a simple, practical way.

Can You Improve PCOS by
Fixing Your Metabolism?
This is where many women start to see a meaningful shift.
While PCOS is a complex condition, addressing metabolic health - particularly insulin resistance - can have a significant impact on symptoms.
In clinical settings, improving metabolic function is often associated with:
- More regular menstrual cycles
- Reduced cravings and improved energy
- Easier weight management
- Improvements in skin and hormonal symptoms
It’s important to note that this is not about a quick fix or a one-size-fits-all solution.
However, for many women, targeting the metabolic drivers of PCOS creates a much more effective and sustainable path forward than focusing on symptoms alone.
Practical Steps to
Start Improving Your Metabolic Health
If you’re feeling overwhelmed, the most important thing is to start simple.
You don’t need to overhaul everything at once. In fact, small, consistent changes are often what create the most sustainable improvements.
Here are a few practical starting points:

Build Your Meals Around Protein
Aim to include a quality source of protein at each meal. This helps stabilise blood sugar, improve satiety, and support metabolic function.

Avoid Long Gaps Between Meals
Going too long without eating can lead to blood sugar dips, which often trigger cravings and energy crashes later in the day.

Reduce Highly Processed Foods
Focus on whole, minimally processed foods where possible. These tend to have a more stable impact on blood sugar and overall metabolism.

Pay Attention to Energy and Hunger Signals
Your body provides useful feedback. Noticing patterns in your energy, cravings, and hunger can help guide what adjustments are needed.

Focus on Consistency, Not Perfection
Metabolic health improves through repeated daily habits - not extreme short-term efforts.
Summary:
Understanding PCOS and Metabolism
PCOS is not just a hormonal condition - it is closely linked to how the body regulates energy, blood sugar, and insulin.
For many women, underlying metabolic dysfunction - particularly insulin resistance - is a key driver of symptoms such as weight gain, fatigue, and hormonal imbalance.
The most effective approach is not simply to “eat less” or “exercise more,” but to support the body’s metabolic processes in a targeted and sustainable way.
By improving metabolic health, it becomes possible to:
- Stabilise energy levels
- Reduce cravings
- Support hormone balance
- Make progress feel more achievable and consistent
When to Seek Professional Support
While many women can make meaningful progress with the right foundational changes, there are times when more personalised support is helpful.
You may benefit from professional guidance if:
- Symptoms are persistent despite your efforts
- You feel unsure how to structure your nutrition
- You suspect significant insulin resistance
- You want a clear, tailored plan rather than trial and error
Working with a practitioner who understands the metabolic side of PCOS can help you:
- Identify what’s driving your symptoms
- Implement a structured, evidence-based approach
- Avoid common pitfalls that slow progress
If you’re looking for a more personalised approach, you can learn more about working together through my clinical nutrition programs.
[Button: Work With Me]
Start Improving Your Metabolic Health Today
If you’re ready to take a more structured and effective approach to managing PCOS, the first step is understanding how to support your metabolism properly.
Download the PCOS Metabolic Reset Guide.
Inside, you’ll learn:
- How to structure your meals for stable blood sugar
- The key drivers behind PCOS symptoms
- Practical steps you can start immediately
