Start Here: Reset Your Metabolism
If you want a structured starting point, download our free 7-day metabolic reset guide.
A simple, clinically-informed plan to help stabilise blood sugar, improve metabolism, and reduce common PCOS symptoms.

What Is Insulin Resistance?
Insulin resistance occurs when the body’s cells become less responsive to insulin, a hormone responsible for regulating blood sugar levels.
Under normal conditions:
- You eat → blood glucose rises
- Insulin is released → glucose is transported into cells
- Blood sugar returns to a stable level
However, when insulin resistance develops, this process becomes less efficient.
Cells do not respond as effectively to insulin’s signal, meaning:
- More insulin is required
- Blood insulin levels remain elevated
- Glucose regulation becomes less stable
This state is often referred to as hyperinsulinaemia - where insulin levels are chronically higher than optimal.
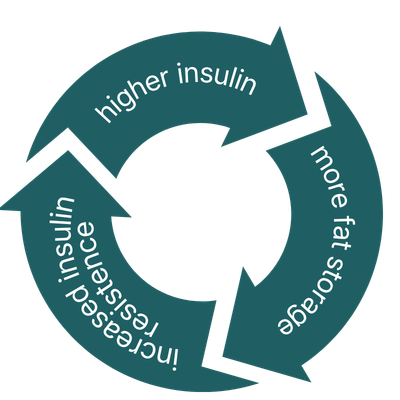
Over time, this can contribute to:
- Increased fat storage
- Disrupted hunger signals
- Reduced metabolic flexibility
Importantly, insulin resistance can exist for years before showing up on standard blood tests, which is why many women experience symptoms long before receiving any diagnosis.
What Does Insulin Do in the Body?
Insulin is often described simply as a “blood sugar hormone,” but its role is much broader.
It acts as a key regulator of energy metabolism, influencing how the body uses, stores, and distributes fuel.
Its primary functions include:
- Glucose regulation: helping move glucose from the bloodstream into cells
- Energy storage: promoting storage of excess glucose as glycogen or fat
- Fat metabolism: influencing whether the body burns fat or stores it
- Appetite regulation: indirectly affecting hunger and satiety signals
When insulin is functioning well, the body can efficiently switch between using glucose and stored fat for energy - a process known as metabolic flexibility.
In insulin resistance, this flexibility becomes impaired.
The body becomes more reliant on glucose, less efficient at burning fat, and more prone to storing energy.
What Causes Insulin Resistance?
Insulin resistance is rarely caused by a single factor.
It typically develops gradually in response to a combination of dietary, lifestyle, and hormonal influences.
Frequent Blood Sugar Spikes
Regular consumption of highly refined carbohydrates and sugars can lead to repeated spikes in blood glucose.
Over time, this places increased demand on insulin production, contributing to reduced sensitivity.
Chronic Stress and Cortisol
Stress hormones such as cortisol can increase blood sugar levels and interfere with insulin signalling.
When stress is ongoing, this can contribute to persistent metabolic disruption.
Low Protein and Fibre Intake
Meals lacking protein and fibre are digested more quickly, leading to sharper increases in blood sugar.
This can drive higher insulin responses over time.
Physical Inactivity
Skeletal muscle plays a major role in glucose uptake.
Lower levels of physical activity can reduce the body’s ability to utilise glucose efficiently.
Hormonal Influences
Insulin resistance is strongly linked with hormonal conditions, particularly:
- PCOS
- Perimenopause
Hormonal shifts can alter how the body responds to insulin, making metabolic regulation more challenging.
Common Signs of Insulin Resistance
Insulin resistance does not always present with obvious or severe symptoms, which is why it is often overlooked.
However, there are several patterns that commonly emerge.
-
- Persistent fatigue or low energy
- Cravings for sugar or refined carbohydrates
- Energy crashes after meals
- Difficulty losing weight despite effort
- Increased abdominal fat storage
- Brain fog or reduced concentration
- Feeling hungry soon after eating
- Irritability when meals are delayed
These symptoms are often linked to underlying instability in blood sugar regulation.
For example, a rapid rise in blood sugar followed by a sharp drop can create cycles of energy fluctuation, cravings, and hunger.
Recognising these patterns is important, as they provide insight into how the body is responding metabolically.
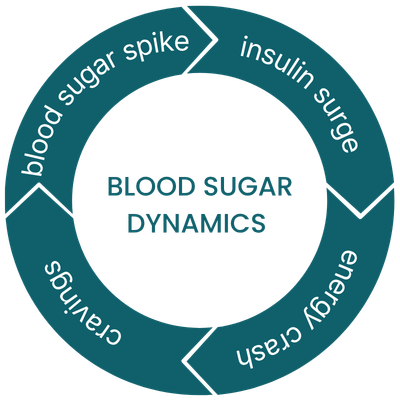
How Insulin Resistance Affects Blood Sugar
To understand insulin resistance, it helps to look at what happens after eating.
When a meal—particularly one high in refined carbohydrates—is consumed:
- Blood glucose rises quickly
- Insulin is released to manage this increase
In insulin resistance:
- A larger amount of insulin is required
- Blood sugar may drop more rapidly afterwards
- This can trigger hunger and cravings
Over time, this creates a repeating cycle: Blood sugar spike → insulin surge → energy crash → cravings
This cycle not only affects energy and appetite, but also reinforces the underlying metabolic imbalance.
If this cycle feels familiar…
Download the Metabolic Reset Guide to learn how to stabilise your blood sugar step-by-step.
Health Conditions Linked to Insulin Resistance
Insulin resistance is a key underlying driver in several common health conditions, particularly in women.
These include:
- Polycystic Ovary Syndrome (PCOS)
- Weight gain and difficulty losing weight
- Prediabetes and type 2 diabetes
- Fatigue and energy dysregulation
In many cases, addressing insulin resistance can lead to improvements across multiple symptoms simultaneously.
How to Improve Insulin Resistance
One of the most important things to understand is that insulin resistance is highly modifiable.
Rather than focusing on restriction, the goal is to support the body’s ability to regulate blood sugar more effectively.
1. Structure Meals to Stabilise Blood Sugar
Including protein, healthy fats, and fibre in each meal helps slow glucose absorption and reduce insulin spikes.
2. Prioritise Protein Intake
Protein supports satiety, muscle maintenance, and metabolic activity.
3. Choose Carbohydrates Strategically
Focusing on whole, minimally processed carbohydrate sources can improve blood sugar stability.
4. Improve Meal Timing and Consistency
Regular eating patterns can help reduce large fluctuations in blood sugar.
5. Support Lifestyle Foundations
Sleep, stress management, and movement all play important roles in insulin sensitivity.
If you want a clear structure to follow...
Can Insulin Resistance Be Reversed?
In many cases, insulin resistance can be significantly improved—and sometimes effectively reversed—through consistent, targeted strategies.
The key is addressing the underlying drivers rather than focusing only on symptoms.
This includes:
- Stabilising blood sugar
- Reducing chronically elevated insulin levels
- Supporting metabolic flexibility
Progress is typically gradual, but meaningful improvements can occur over time.
Practical Steps to
Start Improving Your Insulin Sensitivity
If you’re feeling overwhelmed, the most important thing is to start simple.
You don’t need to overhaul everything at once. In fact, small, consistent changes are often what create the most sustainable improvements.
Here are a few practical starting points:

Build Your Meals Around Protein
Aim to include a quality source of protein at each meal. This helps stabilise blood sugar, improve satiety, and support metabolic function.

Avoid Long Gaps Between Meals
Going too long without eating can lead to blood sugar dips, which often trigger cravings and energy crashes later in the day.

Reduce Highly Processed Foods
Focus on whole, minimally processed foods where possible. These tend to have a more stable impact on blood sugar and overall metabolism.

Pay Attention to Energy and Hunger Signals
Your body provides useful feedback. Noticing patterns in your energy, cravings, and hunger can help guide what adjustments are needed.

Focus on Consistency, Not Perfection
Metabolic health improves through repeated daily habits - not extreme short-term efforts.
Summary:
Understanding Insulin Resistance
Insulin resistance is a common but often overlooked driver of metabolic dysfunction.
It affects how the body regulates blood sugar, stores energy, and responds to food.
By improving insulin sensitivity, it becomes possible to:
- Stabilise energy levels
- Reduce cravings
- Support weight management
- Improve overall metabolic health
When to Seek Professional Support
While general strategies can be effective, some women benefit from more personalised guidance.
This is particularly true if symptoms are persistent or progress feels unclear.
Working with a practitioner can help:
- Identify underlying drivers
- Create a tailored plan
- Provide structure and accountability
If you’re looking for a more personalised approach, you can learn more about working together through my clinical programs.
Start Improving Your Metabolic Health Today
If you’re ready to take a more structured and effective approach toward improving insulin sensitivity, understand how to support your metabolism properly.
Download the Metabolic Reset Guide.
Inside, you’ll learn:
- How to structure your meals for stable blood sugar
- The key drivers behind insulin sensitivity
- Practical steps you can start immediately
