Introduction
If you have PCOS and acne, there is a very good chance you have spent years treating your skin without anyone adequately treating the reason your skin is breaking out in the first place.
Topical creams. Antibiotics. Hormonal contraceptives. Perhaps even Roaccutane. Each one may have worked - for a while - and then stopped, or required ongoing use just to maintain results. The moment you stopped, the acne came back.
This is not a skin problem. It is a hormonal and metabolic problem that shows up on your skin.
PCOS-related acne is driven by elevated androgens, which are themselves driven by insulin resistance and chronic inflammation - the same mechanisms at the root of most PCOS symptoms. Until those underlying drivers are addressed, the skin is simply responding to an internal environment that continues to generate the conditions for acne regardless of what you apply topically or take short-term.
This article explains that mechanism clearly - and what a genuinely root-cause approach to PCOS acne actually looks like.
Why PCOS Causes Acne: The Hormonal Chain
To understand why PCOS causes acne, you need to understand what androgens do to the skin - and why women with PCOS tend to have elevated androgens in the first place.
Androgens and the Skin
Androgens - testosterone and its more potent derivative DHT (dihydrotestosterone) - have direct effects on the sebaceous glands in the skin. These are the glands responsible for producing sebum, the oily substance that lubricates and protects the skin.
In normal amounts, sebum production is entirely appropriate. The problem arises when androgens are elevated and sebaceous gland activity is driven beyond what the skin can manage:
- Sebum production increases significantly, creating an oilier skin environment
- The cells lining the hair follicle (keratinocytes) proliferate more rapidly and shed less efficiently, causing follicle blockage
- Blocked follicles trap sebum and dead skin cells, creating the environment in which Cutibacterium acnes (the bacteria associated with acne) thrives
- The immune system responds to bacterial proliferation with localised inflammation - producing the red, inflamed, sometimes painful lesions characteristic of hormonal acne
This is why hormonal acne in PCOS tends to be deeper, more inflamed, and more resistant to topical treatment than the surface-level comedonal acne common in adolescence. It is being driven from the inside - by an hormonal signal that topical products simply cannot reach.
Where Do Elevated Androgens Come From in PCOS?
In PCOS, androgen excess is primarily driven by two interconnected factors: elevated insulin and chronic inflammation.
Elevated insulin directly stimulates androgen production. The ovaries have insulin receptors, and when insulin levels are chronically high - as they are in insulin-resistant PCOS - the ovaries respond by producing more testosterone and androstenedione. At the same time, high insulin suppresses sex hormone-binding globulin (SHBG) - the protein that binds testosterone in the bloodstream and renders it inactive. Less SHBG means more free, biologically active testosterone circulating in the body.
The result: more testosterone being produced, less of it being bound and neutralised, and more of it reaching androgen receptors in the skin.
Chronic inflammation amplifies androgen production. As covered in PCOS and Inflammation: The Hidden Driver Behind Your Symptoms, inflammatory chemicals directly signal the ovaries to produce more androgens. This is why factors that seem entirely unrelated to your skin - poor sleep, chronic stress, a high-sugar diet, gut dysbiosis - can trigger or worsen acne flares. They are raising your inflammatory load, which raises your androgen output, which drives your skin to break out.
For the foundational explanation of how insulin drives androgen excess in PCOS: High Insulin and PCOS: Why It Disrupts Hormones
Insight
PCOS acne is not a skin condition. It is a metabolic and hormonal condition with a cutaneous presentation. This distinction matters enormously for treatment. Approaches that target the skin surface can manage symptoms temporarily, but they cannot resolve the hormonal signal that is generating those symptoms. That signal originates in your insulin levels, your inflammatory environment, and your androgen production - and it responds to interventions at that level.
Recognising Hormonal Acne in PCOS
PCOS-related acne has a recognisable pattern that distinguishes it from other types of acne. Understanding whether your acne fits this profile helps clarify whether the hormonal and metabolic root cause framework is the right lens for your situation.
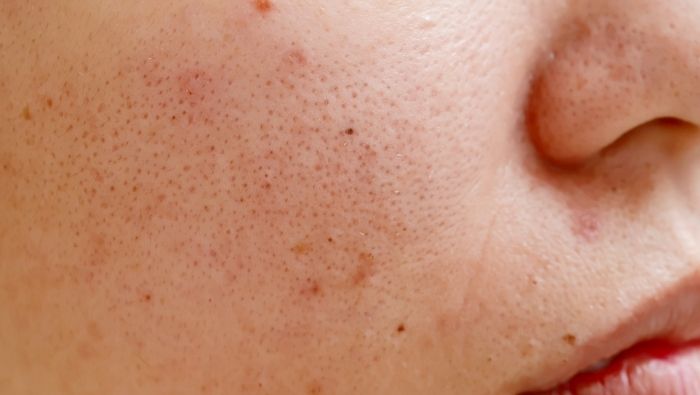
Location: Hormonal acne in PCOS is predominantly found on the lower face - the jawline, chin, and lower cheeks. This distribution reflects the higher density of androgen-sensitive sebaceous glands in these areas. Chest and back acne is also common in PCOS. Forehead and nose acne (the classic T-zone) is less specifically associated with androgen excess.
Type of lesions: PCOS acne tends toward deeper, cystic, or nodular lesions rather than surface-level blackheads and whiteheads. These deeper lesions are more painful, take longer to resolve, and are more likely to leave post-inflammatory hyperpigmentation (dark marks) or scarring.
Cyclical pattern: Many women with PCOS notice that acne worsens at predictable points in the cycle - typically in the days before menstruation, when androgens are relatively higher. However, because PCOS often involves elevated androgens throughout the cycle rather than just perimenstrually, some women experience persistent rather than cyclical acne.
Resistance to standard treatments: If your acne has not responded adequately - or has only responded temporarily - to conventional treatments including topical retinoids, benzoyl peroxide, oral antibiotics, or even the oral contraceptive pill, this is clinically significant. It suggests the underlying hormonal driver has not been adequately addressed.
Associated PCOS features: Acne occurring alongside other androgen-related symptoms - excess facial or body hair, scalp hair thinning, irregular periods, weight gain around the abdomen - strengthens the case for a hormonal root cause.
Why Common Acne Treatments Fall Short in PCOS
Understanding why standard treatments produce limited or temporary results in PCOS acne helps clarify what a more complete approach needs to include.
Topical Treatments
Topical products - retinoids, benzoyl peroxide, salicylic acid, niacinamide - can reduce bacterial load, improve skin cell turnover, and manage surface oil to a degree. They are not without value, and many women with PCOS use them as part of a broader approach.
But they cannot reach the sebaceous glands at the depth at which androgen-driven stimulation is occurring, and they cannot alter the hormonal signal that is driving sebum overproduction. When the topical treatment is discontinued, the hormonal environment that was generating the acne remains unchanged.
Oral Antibiotics
Antibiotics reduce C. acnes bacterial load and have anti-inflammatory properties that can suppress active lesions. Many women see good results initially. The problem is that they address a downstream consequence - bacterial proliferation - rather than the upstream driver - androgen-stimulated sebum excess. When antibiotics are stopped, bacterial populations recover and acne typically returns.
There are also legitimate concerns about the long-term impact of repeated antibiotic courses on gut microbiome diversity - which, as discussed in PCOS and Inflammation, has its own consequences for systemic inflammation and metabolic health.
The Oral Contraceptive Pill
The pill is frequently prescribed for PCOS acne and often works well during the period of use. Oestrogen in combined oral contraceptives raises SHBG - binding more testosterone and reducing free androgen activity. Some pill formulations also contain progestins with anti-androgenic properties that directly reduce androgen receptor activity in the skin.
For some women, the pill is an appropriate and effective part of their overall PCOS management. The clinical consideration is that it suppresses the hormonal expression of PCOS without addressing the underlying metabolic drivers. When the pill is stopped - for any reason, including wanting to conceive - the acne frequently returns because the insulin resistance and inflammatory load that were driving androgen excess throughout have not been addressed.
This is not an argument against the pill. It is an argument for addressing the metabolic root alongside any pharmaceutical management.
Roaccutane (Isotretinoin)
Isotretinoin is the most powerful acne treatment available and produces dramatic results in many patients. It works by permanently reducing sebaceous gland size and sebum output.
In women with PCOS, however, the hormonal drive to sebum overproduction remains after treatment - and for some women, acne recurs because the glands, though reduced, are still being overstimulated by elevated androgens. Recurrence rates after isotretinoin in women with underlying hormonal acne are higher than in non-hormonal acne, and some women require repeat courses.
Again - not an argument against isotretinoin where it is clinically appropriate. An argument for addressing the underlying hormonal and metabolic environment that is driving the condition.
Insight
There is nothing wrong with using topical treatments, antibiotics, the pill, or even isotretinoin to manage PCOS acne - these have real clinical value and can provide meaningful relief while the deeper work is being done. The issue is treating them as the complete solution when they are, at best, symptomatic management. The most robust and durable outcomes come from combining appropriate skin-directed treatments with a genuine metabolic approach that addresses insulin resistance and inflammatory load at the root.
The Diet–Acne Connection in PCOS
The relationship between diet and acne has historically been dismissed in dermatology - the "chocolate causes acne" claim was debunked, and with it, dietary consideration largely fell out of mainstream acne management.
The research landscape has shifted significantly. And for women with PCOS specifically, the connection between dietary pattern, insulin response, and acne severity is now well-supported.¹
High-Glycaemic Diets and Acne
Multiple clinical trials have demonstrated that high-glycaemic diets - characterised by refined carbohydrates, sugars, and foods that drive rapid blood glucose spikes - worsen acne. The mechanism is directly relevant to PCOS:
High-glycaemic eating raises blood glucose → raises insulin → insulin stimulates IGF-1 (insulin-like growth factor 1) production → IGF-1 acts synergistically with androgens to stimulate sebum production and keratinocyte proliferation → more follicle blockage and more sebum = more acne.
IGF-1 also directly suppresses SHBG - the protein that binds and neutralises testosterone - further amplifying the androgenic drive to the skin.
A landmark study found that young men following a low-glycaemic diet for 12 weeks had significantly fewer acne lesions and lower androgen levels compared to those on a high-glycaemic diet.² The mechanism applies equally to women with PCOS, and more acutely - because insulin resistance means the insulin and IGF-1 response to high-glycaemic food is already amplified above baseline.
Dairy and Acne
The dairy–acne connection is more nuanced and the research less definitive, but it is worth understanding in the context of PCOS. Cow's milk - particularly skim milk - has a disproportionately high insulinogenic effect relative to its glycaemic index. It also contains IGF-1 directly, as well as precursors that stimulate IGF-1 production in the body.
For women with PCOS who are already managing elevated insulin and insulin-like signalling, a high dairy intake may be contributing to androgenic skin stimulation through this pathway. The evidence does not support removing all dairy universally - but for women with PCOS whose acne is not responding despite other interventions, reducing dairy intake, particularly skim and low-fat dairy products, is a reasonable evidence-informed trial.
Omega-3 Fatty Acids and Skin Inflammation
Omega-3 fatty acids - found in oily fish, walnuts, flaxseed, and chia seeds - have direct anti-inflammatory effects on sebaceous gland activity. Research shows that higher omega-3 intake is associated with reduced acne severity, and supplementation produces measurable reductions in inflammatory acne lesions.³
Given that PCOS acne is, at its core, an inflammatory process in the skin driven by an inflammatory hormonal environment, this is a particularly relevant nutritional intervention. The approach to omega-3 intake recommended for PCOS inflammation generally covers the dose required for skin benefit as well.
A simple practical test of the dietary–acne link is to notice whether your skin worsens in the days following periods of higher sugar or refined carbohydrate intake - stress eating, holidays, celebrations. For many women with PCOS, this pattern is clear once they are looking for it. It is not definitive evidence, but it is useful personal data that supports the decision to prioritise blood sugar management as part of your skin approach.
How Managing Insulin Resistance Improves PCOS Acne
When insulin resistance is genuinely addressed - through diet, movement, and targeted nutritional support - the downstream effects on PCOS acne can be significant:
- Insulin levels fall → IGF-1 activity reduces → less sebum stimulation
- SHBG rises → more free testosterone is bound and neutralised → reduced androgenic drive to the skin
- Ovarian androgen production decreases → lower circulating testosterone and DHT
- Inflammatory load reduces → less inflammatory signalling in sebaceous glands → less severe and less frequent lesions
These changes do not happen overnight. Hormonal shifts driven by metabolic improvement typically become visible over two to four months - the timeframe of the hair follicle and sebaceous gland cycle. This is important to hold in mind: meaningful improvement in PCOS acne through a metabolic approach takes time, and that timeline is physiological, not a reflection of whether the approach is working.
The clinical trajectory tends to follow this pattern: reduction in new active lesions first, then gradual improvement in existing inflammatory lesions, then improvement in post-inflammatory marks over subsequent months.
For the foundational dietary approach to insulin resistance in PCOS: Best Diet for PCOS and Insulin Resistance and How to Balance Blood Sugar with PCOS
Stress, Sleep, and Your Skin
Two factors that significantly worsen PCOS acne - and that are frequently overlooked entirely in skin-focused treatment plans - are chronic stress and poor sleep.
Cortisol and sebum production: Cortisol directly stimulates sebaceous gland activity and increases sebum output - independently of androgen levels. This is one mechanism by which stress flares acne even in women who do not have PCOS. In women with PCOS, where cortisol dysregulation is already common, this effect is amplified. The worsening of acne during periods of high stress is not imagined - it is a direct physiological response.
Sleep deprivation and skin inflammation: Poor sleep raises cortisol, elevates inflammatory markers, and impairs the skin's barrier function and overnight repair processes. The skin does significant regenerative work during sleep - cell turnover, collagen synthesis, barrier repair. Chronic sleep deprivation disrupts this cycle, increasing inflammatory acne severity and slowing the resolution of existing lesions.
For the full clinical picture of cortisol in PCOS: Cortisol and PCOS: The Stress–Blood Sugar Connection And for sleep: PCOS and Sleep: Why Poor Sleep Worsens Insulin Resistance
Addressing stress physiology and sleep quality is genuinely part of a complete PCOS acne management approach - not because stress management is vaguely good for you, but because cortisol is a direct driver of the sebaceous gland activity underlying your breakouts.
A Note on Skincare in PCOS
While systemic intervention addresses the root cause, appropriate skincare supports the skin during the process and can meaningfully reduce severity and scarring.
For PCOS acne, the evidence broadly supports:
Gentle, non-stripping cleansing. Over-cleansing and harsh products disrupt the skin barrier, triggering compensatory sebum production and worsening inflammatory acne. A mild, non-comedogenic cleanser used twice daily is sufficient.
Topical retinoids. Vitamin A derivatives (tretinoin, adapalene) improve follicular cell turnover, reduce comedone formation, and have anti-inflammatory properties. They are among the best-evidenced topical treatments for hormonal acne and work well as part of a combined approach.
Niacinamide. Vitamin B3 reduces sebum production, improves skin barrier function, and has meaningful anti-inflammatory properties. It is well-tolerated by most skin types and is a useful addition to a PCOS-oriented skincare routine.
Sun protection. Daily broad-spectrum SPF is non-negotiable if you are using retinoids (which increase photosensitivity) and is critically important for preventing the worsening of post-inflammatory hyperpigmentation - the dark marks left by PCOS acne that can linger for months.
What to avoid: physical scrubbing, alcohol-based products, and anything that strips the skin - all of which compromise the skin barrier and worsen the inflammatory environment locally.
If you are working on your PCOS metabolically and using appropriate skincare simultaneously, give the combined approach a minimum of three to four months before evaluating results. Skin improvement in response to hormonal changes operates on the timescale of the follicular cycle - not weeks. Impatience at the two-month mark often leads women to abandon an approach that would have produced meaningful change by month four.
Clinical Insight
The relationship between PCOS, insulin resistance, androgen excess, and acne is well-established in the clinical and dermatological literature. Elevated insulin drives ovarian androgen production and suppresses SHBG, increasing free testosterone activity at androgen receptors in the sebaceous glands. Chronic inflammation amplifies this process at multiple points in the hormonal cascade. The evidence for dietary glycaemic load as a modifiable driver of acne severity is now substantial - clinical trials consistently show that lowering dietary glycaemic load reduces both acne lesion count and circulating androgen levels. For women with PCOS, this is not an alternative approach - it is the mechanistically appropriate first-line metabolic intervention, best used alongside, not instead of, dermatological management where that is clinically indicated.
The Bottom Line
PCOS acne keeps coming back because most treatments address the skin without addressing the hormonal and metabolic environment that is generating the acne in the first place.
That environment - elevated insulin, androgen excess, chronic inflammation, cortisol dysregulation - is the target. When it shifts, the skin follows. The timeline is measured in months, not weeks, because hormonal change operates on a biological cycle. But the results, when driven by genuine metabolic improvement, tend to be durable in a way that topical and pharmaceutical management alone rarely achieves.
This does not mean abandoning your skincare or your dermatologist. It means understanding that the most complete and lasting approach to PCOS acne works on both levels simultaneously - managing the skin surface while addressing the metabolic root that is driving everything from the inside.
Your skin is not the problem. It is reflecting one.
Ready to Address the Metabolic Root of Your PCOS Symptoms?
In my clinic, I work with women to address the insulin resistance, inflammatory load, and hormonal dysregulation that drive PCOS symptoms - including acne that has not responded adequately to conventional treatment.
Our metabolic programs use your individual blood chemistry to design a personalised nutrition protocol that works to recalibrate insulin sensitivity, reduce androgen-driving inflammation, and restore hormonal balance from the inside.
Women commonly report improvements in skin clarity as one of the earlier and more motivating changes they notice through the programme - typically emerging alongside improvements in energy, cravings, and cycle regularity as the metabolic environment begins to shift.
Working with women in-clinic and remotely. If your skin - and your PCOS - deserve a root cause approach, we are here for that conversation.
Free Resource - Start Here
Want to start shifting your metabolic environment right now?
The 7-Day Metabolic Reset is a free, structured guide built for women with PCOS and insulin resistance. It covers blood sugar stabilisation, anti-inflammatory nutrition, cortisol support, and practical daily strategies - all in a clear, seven-day framework.
👉 Download the 7-Day Metabolic Reset
Clinically grounded. No gimmicks. A genuine starting point for working with your biology rather than against it.
References
- Burris J, et al. (2013). Acne: the role of medical nutrition therapy. Journal of the Academy of Nutrition and Dietetics, 113(3), 416–430.
- Smith RN, et al. (2007). A low-glycemic-load diet improves symptoms in acne vulgaris patients: a randomized controlled trial. American Journal of Clinical Nutrition, 86(1), 107–115.
- Khayef G, et al. (2012). Effects of fish oil supplementation on inflammatory acne. Lipids in Health and Disease, 11, 165.
- Melnik BC, et al. (2011). Role of insulin, insulin-like growth factor-1, hyperglycaemic food and milk consumption in the pathogenesis of acne vulgaris. Experimental Dermatology, 20(10), 781–788.
- Tasli L, et al. (2013). Insulin-like growth factors in patients with acne vulgaris. Journal of the European Academy of Dermatology and Venereology, 27(6), 769–773.